Your skin’s been breaking out. Not all over — just where your mask sits. The chin. The jaw. Maybe around the nose or across the cheeks. Everything else in your life is the same as it’s always been, this may be related to mask use.
You’re probably dealing with maskne. Maskne is a recognised skin condition associated with prolonged mask use.
So what does maskne actually mean?
Mask plus acne. That’s the maskne meaning in its simplest form. But it’s a bit more specific than just "pimples from wearing a mask."
The medical term is acne mechanica — a type of breakout caused by physical factors rather than the hormonal or bacterial reasons most people associate with acne. When a mask presses against your face, it seals in heat, moisture, and oil. Your breath sits in that warm little pocket between the fabric and your skin. Sweat builds up. Pores may become blocked more easily. And bacteria may proliferate in this environment.
The result? Breakouts that map almost exactly to your mask zone. Jaw, chin, sides of the nose, lower cheeks — wherever the mask sits, that’s where maskne shows up. These are common areas where maskne may occur.
Is maskne real, though, or did the internet just make up a catchy word? It’s real. Dermatologists were treating it in healthcare workers long before COVID made masks part of everyday life. It’s documented in peer-reviewed medical literature. It made it into the Merriam-Webster dictionary in 2021. It is recognised within dermatology literature.
Who actually gets it?
Short answer: anyone who masks regularly. But some people are a lot more prone to it than others.
If you’ve always had oily or acne-prone skin, you may be at increased risk. The excess sebum that’s already sitting in your pores may be more prone to blockage and inflammation — add a warm, humid mask environment and it happens faster.
Makeup is another big one. Foundation under a mask may contribute to pore blockage under occlusion. It mixes with heat and sweat, breaks down, and ends up sitting in your pores in a way it wouldn’t out in the open air. A lot of people who thought their maskne had appeared randomly were masking over a full face of foundation every single day.
Nurses and healthcare workers have dealt with this the longest and the worst. Wearing N95 respirators across a ten-hour shift — sometimes double-masked — is a very different experience from wearing a cotton mask at the shops. Prolonged occlusion may increase irritation and congestion. The occlusion is intense. Many nurses were developing it years before most of us had ever heard the term.
It’s worth knowing, too, that maskne doesn’t always look like typical pimples. Some people develop perioral dermatitis — a rash that clusters around the mouth and nose. Others get rosacea flares triggered by the heat under the mask, or folliculitis where the hair follicles get infected. And if you’re reacting to the mask material itself — certain surgical masks contain chemicals that can cause contact dermatitis along the edges — that’s a different skin condition with overlapping features, though it can look similar.
How long does maskne last?
This varies between individuals and what they do about it.
For mild cases — a few new pimples that appeared after you started masking more — two to three weeks of adjusted skincare and a cleaner mask habit may be sufficient in some cases. It doesn’t always need products or treatment. Sometimes it’s just about removing the trigger.
For people wearing masks all day, every day — healthcare workers, retail staff, tradespeople — maskne can linger for months if nothing changes. The skin keeps getting exposed to the same conditions and may persist if contributing factors remain unchanged.
Four to six weeks is a fair window to try managing it at home. If you’re not seeing improvement by then, or if the breakouts are painful, deep, or spreading, that’s the point to seek professional assessment and get a professional to look at it.
Maskne prevention — The part most people skip
Maskne prevention may be managed with consistent skincare and hygiene measures, but it does require a bit of consistency.
The face mask for maskne-prone skin can influence skin irritation and breakouts. A 100% cotton mask breathes better than anything synthetic and causes less friction. Silk-lined masks are even kinder on skin that tends to react. Anything rough, polyester-heavy, or tight-fitting may worsen symptoms — particularly in warmer, more humid climates where sweat and heat under the mask compound the problem faster.
Wash your mask after every wear. One day’s use is enough to accumulate oil, bacteria, and dead skin cells — exactly what you’re trying to keep off your face. Use fragrance-free detergent, skip the fabric softener, and let it dry fully before wearing it again.
Put your mask on over a clean face.It sounds too simple, but masking over yesterday’s moisturiser, this morning’s SPF, or a fresh coat of foundation may increase pore blockage. Clean skin first, every time.
And moisturise before you mask — even if your skin is oily. A thin, non-comedogenic moisturiser acts as a barrier between your skin and the fabric. Ceramide-based formulas are a solid choice. They reinforce the skin barrier without adding anything that’ll block pores.
Take mask breaks when you can. Even stepping outside for ten minutes in fresh air may help reduce heat and moisture buildup.
For nurses: Maskne prevention is a different challenge
If taking your mask off isn’t an option — which, for most healthcare workers, it isn’t for the bulk of a shift — the goal shifts from avoiding the mask to building your skin up so it can handle the exposure better.
Start with a gentle, non-foaming cleanser morning and night, one that removes everything without stripping your skin barrier, because an intact barrier may help support skin barrier function. Before you put your mask on, apply a lightweight moisturiser with niacinamide or ceramides. Niacinamide in particular may be beneficial in some cases — it regulates oil production and calms inflammation, which may assist with oil regulation and inflammation when your face is about to spend eight hours under a respirator.
After your shift, cleanse as soon as you reasonably can. And be careful with actives. Reaching for the retinol after a long shift on skin that’s already been stressed and may increase irritation. Let your skin settle overnight. There’ll be a better time for the stronger stuff.
How to treat maskne: Products, options, and what to know
How to treat maskne depends a lot on what type you’re dealing with — which sounds like a cop-out but genuinely isn’t.
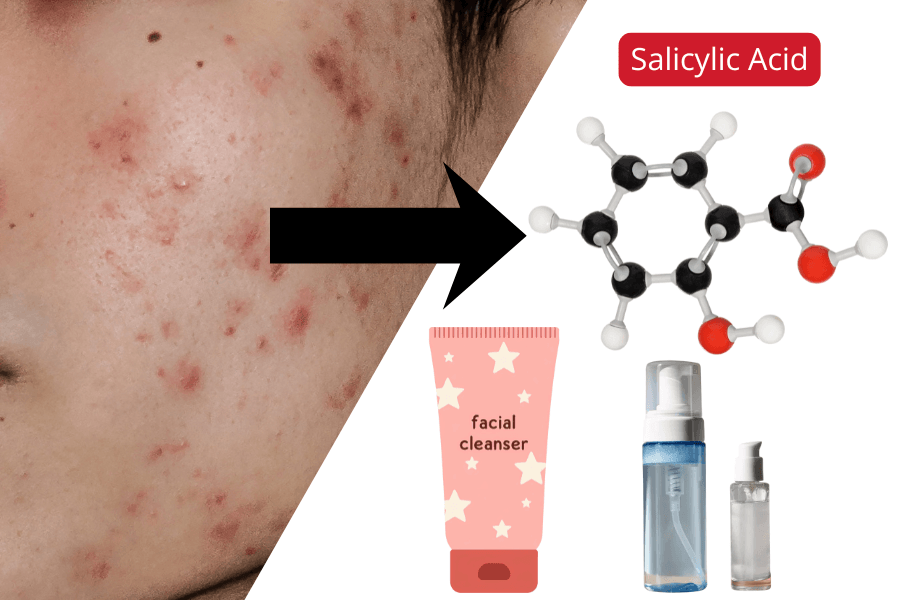
For standard maskne breakouts, salicylic acid is usually the first thing worth trying. It works inside the pore rather than just on the surface, which makes it well-suited to the kind of deep blockages maskne tends to cause. A salicylic acid cleanser or toner, used consistently, may be effective for some people. Benzoyl peroxide helps when there’s a strong bacterial component — just start low (2.5–5%) because combined with mask friction, higher concentrations can increase irritation in some cases .
Niacinamide serums are good to layer in alongside a treatment product. They won’t clear existing breakouts at speed, but they reduce redness and regulate sebum, which may support gradual improvement and makes the skin more resilient over time.
When it comes to maskne products specifically, the key thing to look for is texture. Anything heavy gets compressed under a mask and makes the occlusion problem worse. Maskne gel formulas absorb fast and sit lightly on the skin. A maskne face spray can help midday if your skin needs a reset — aloe vera and centella asiatica are calming ingredients worth looking for, while alcohol and fragrance are worth avoiding.
One consideration is: retinoids and high-strength acids during the day. Under a mask, these get concentrated against the skin by the heat and friction, and the reaction can be worse than the original breakout. Keep retinol at night.
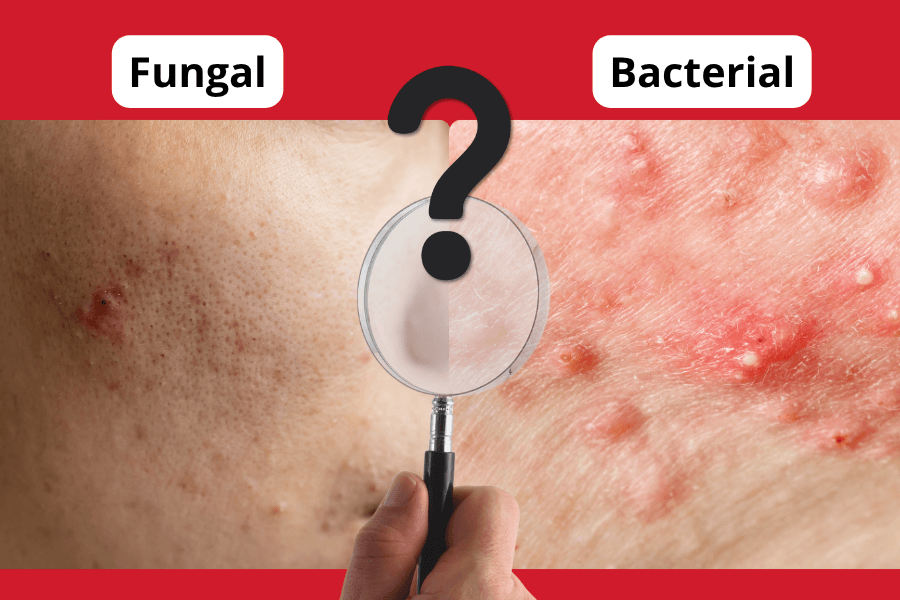
Fungal maskne is worth knowing about because it behaves completely differently. If your maskne looks like small, uniform, itchy bumps rather than typical pimples, it might be fungal acne — caused by yeast overgrowth rather than bacteria. Salicylic acid and benzoyl peroxide may not be effective. You need antifungal treatment, and you need a proper diagnosis before you start trialling multiple products without diagnosis.
Getting telehealth maskne treatment in Australia
If home management isn’t working, the good news is you don’t have to join a months-long waitlist to see a dermatologist.
Telehealth maskne treatment is now well-established in Australia, and telehealth may be suitable for some presentations of maskne. Maskne is largely a visual diagnosis — dermatologists may be able to assess it accurately through high-quality photos and a video call. You upload images beforehand, have the consultation, receive management recommendations tailored to your situation, and if a prescription is needed, it goes straight to your phone as an e-script. Medicare rebates may be available with a valid GP referral.
Services like Acne Express offer after-hours and weekend appointments — something that matters a lot for nurses, shift workers, and anyone whose schedule doesn’t fit neatly around clinic hours.
If you’re in a regional area where getting a specialist appointment quickly is genuinely difficult, telehealth may improve access to care.
The Bottom Line
Getting on top of maskne often involves to a few consistent habits rather than finding the right miracle product. The right face mask for maskne-prone skin. A simple but deliberate routine. Appropriate maskne products when you need them. And professional assessment where needed.
Many people are able to manage mask-related skin concerns with appropriate care. It just needs a bit of backup.
FAQs
Maskne is acne and skin irritation caused by wearing a face mask — “mask” and “acne” pushed together. The maskne meaning goes a bit deeper than just pimples, though. The medical name is acne mechanica. Masks trap heat, moisture, and oil against your skin, which clogs pores and triggers breakouts along your mask line. It can also show up as rashes, folliculitis, or rosacea flares rather than classic pimples, depending on your skin.
Yes. It’s documented in medical literature, widely recognised by dermatologists, and was added to the Merriam-Webster dictionary in 2021. Healthcare workers were reporting it years before most people had heard the term.
Duration varies between individuals. Mild cases — a few new pimples after you started masking more often — can settle in two to four weeks if you sort out your routine early. But if you’re wearing a mask all day for work and nothing changes? It can drag on for months. A lot of people are still dealing with it six months in because they never addressed the root cause. Give home management a solid four to six weeks. If your skin still hasn’t shifted by then, consider seeking professional advice.
A salicylic acid cleanser or toner is a good starting point, alongside a niacinamide serum and a non-comedogenic moisturiser. Maskne gels and sprays help with day-to-day management. If over-the-counter options aren’t making a dent after a few weeks, a dermatologist — in person or via telehealth — may recommend additional treatment options where clinically appropriate.
This is where people tend to overcomplicate things. You don’t need a ten-step routine — several commonly used ingredients may assist in management. Salicylic acid gets into the pore and clears the blockage from within. Niacinamide calms the redness and keeps oil in check. Ceramide moisturisers rebuild whatever the mask friction has been stripping away. Those three, used consistently, cover most cases. Beyond that, maskne gel formulas are worth knowing about — they absorb fast and don’t add to the heaviness under a mask. A maskne face spray with aloe vera or centella asiatica is handy for a midday refresh when you can’t stop for a proper routine. One thing to watch: anything with fragrance or high alcohol content under a mask tends to make irritation worse, not better.
The honest answer is you can’t avoid the exposure — so the goal becomes making your skin tough enough to handle it. That starts with the barrier. A gentle, non-foaming cleanser morning and night, a niacinamide or ceramide moisturiser before every shift, and a proper cleanse the moment you’re done for the day. That routine, done consistently, makes more difference than any fancy product. One thing a lot of nurses get wrong: reaching for retinol or strong actives after a long shift on already-stressed skin. It may increase irritation in some cases. Let your skin breathe overnight first.
Yes — and for something like maskne, telehealth may be a suitable option for some patients. It’s a visual condition. An AHPRA-registered dermatologist can assess it accurately through photos and a video call without you needing to travel anywhere or sit in a waiting room. You upload your skin images beforehand, go through the consultation, and if a prescription’s needed, it lands on your phone as an e-script. Medicare rebates may apply with a GP referral. For nurses or shift workers whose hours make a standard clinic appointment genuinely difficult, this is often a practical access option for some people.
Disclaimer: General information only — not medical advice. For persistent or severe skin concerns, please consult an AHPRA-registered dermatologist or your GP.