You’ve been consistent. You’ve tried the products, stuck to the routine, maybe even seen a doctor. But your skin isn’t clearing — in some cases, symptoms may persist or worsen. Before you blame your hormones or overhaul your entire routine again, consider this: you may be treating a different type of acne than expected.
Not all breakouts are created equal. And the difference between fungal vs bacterial acne isn’t just academic — it can influence treatment choices from which products you use to whether your treatment will help or actively backfire.
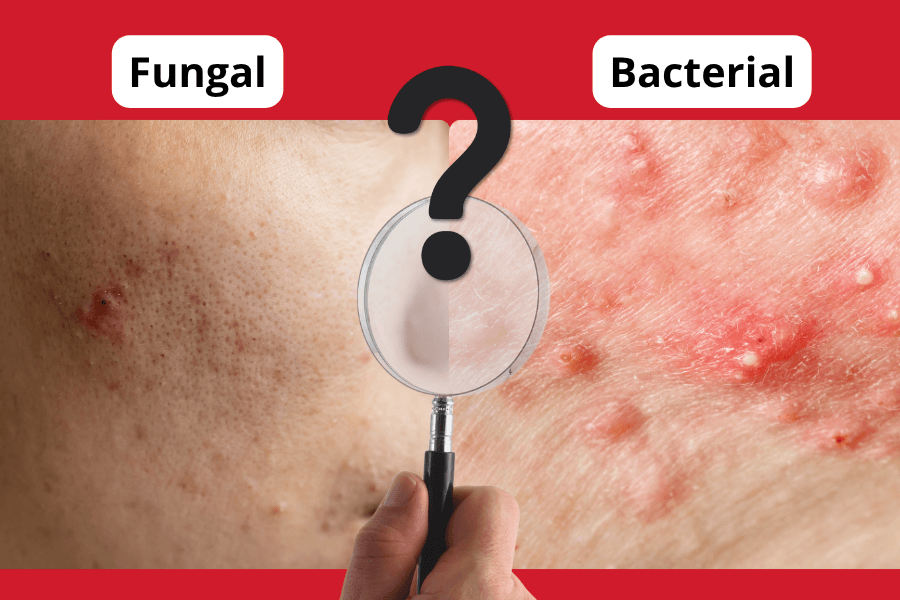
They look alike. That’s the problem.
Both produce red, raised bumps. Both can be inflamed, stubborn, and challenging to manage. So it’s no surprise that people — and in some cases, they may be difficult to distinguish clinically.
But spend a little time with each, and the differences in fungal vs bacterial acne appearance start to show themselves.
Bacterial acne, the kind most people mean when they say "acne," is messy and varied. One week it’s a deep, painful cyst near your chin. The next, it’s a cluster of blackheads across your nose. You might have whiteheads, papules, and nodules all at the same time. It doesn’t follow neat patterns because it’s driven by a complicated mix of hormones, bacteria, excess sebum, and blocked pores.
Fungal acne is different — and tends to present more uniformly. The bumps are small. Consistently small. Usually around 1–2 mm, round, and so uniform in size that they almost appear similar in size and shape. They tend to appear in clusters rather than scattered individually. And here’s the detail that often gets missed: they itch. Not every time, and not dramatically, but enough that it feels distinctly different from a regular pimple. That persistent mild itch may be a helpful distinguishing feature.
Technically, fungal acne is called Malassezia folliculitis — an overgrowth of yeast (Malassezia) that lives on everyone’s skin. Usually it behaves itself. But give it the right conditions — heat, humidity, excess oil, disrupted skin flora — and it colonises the hair follicles and may contribute to symptoms.
Face breakouts: Location is a clue worth following
The difference between fungal acne and bacterial acne on face goes beyond appearance. Where breakouts appear on the face may provide useful clues.
Bacterial acne has a tendency to cluster in oilier zones — the forehead, nose, and chin. Hormonal bacterial acne, specifically, tends to concentrate along the jawline and lower face. Fungal acne, by contrast, commonly affects the forehead and cheeks, and often seems to flare after sweaty days, after wearing heavy or occlusive makeup, or — notably — after a course of antibiotics.
That last point can be confusing. Antibiotics are commonly prescribed for bacterial acne. But they also disrupt the balance of naturally occurring bacteria on the skin, giving Malassezia less competition and more room to flourish. Someone might finish a course of antibiotics for bacterial acne, notice their skin breaking out again, and may assume the treatment was ineffective —when in reality a different problem has emerged.
Looking at fungal vs bacterial acne on cheeks specifically, bacterial cheek acne often links to contact irritation: a phone pressed to the face, an unwashed pillowcase, or habitual touching. The spots tend to be mixed—some comedones, some inflamed papules, distributed in no particular pattern. Fungal cheek breakouts appear more uniform, arriving in clusters of nearly identical bumps. They sometimes spread outward in a way that bacterial acne doesn’t.
Applying heavy, oil-rich products to fungal cheek acne, or continuing antibacterial treatments, may worsen symptoms in some cases. . Both can feed Malassezia.
What the back and body can tell you
Body acne is actually where this whole comparison gets a little easier to navigate — partly because you’re looking at a larger canvas, and partly because the patterns tend to be more obvious when they’re not squeezed into a small section of your face.
Take the back. Bacterial acne is a fairly familiar beast for anyone who’s dealt with it. It’s variable in presentation — a combination of surface-level spots and those deeper, inflamed cystic lesions that sit under the skin and may take longer to resolve . Oily skin, hormones, friction from a gym bag strap, a sweaty workout shirt that stayed on too long — these are the usual suspects.
Fungal back acne may present with a different texture, even if it doesn’t look dramatically different at first. Small bumps, all about the same size, spread across the upper back, shoulders, or chest. Sometimes itchy. Not always, but often enough to notice. And there’s usually a trigger lurking somewhere in recent history — a run of hot, humid weather, a period of heavy exercise without quick showering, a course of antibiotics for something unrelated. These are the conditions Malassezia quietly waits for.
One thing worth trying: run your fingertips lightly over the affected area. Fungal bumps have a texture — a rough one that may feel slightly rough to touch — that bacterial acne usually doesn’t replicate quite the same way.
And if you’re still not sure, ask yourself three things. Are the bumps all roughly the same size? Is there any itching, even mild? Did this start or get noticeably worse after heat, heavy sweating, or antibiotics? If you’re nodding at all three, this may suggest a particular pattern — and may indicate that alternative treatment approaches are needed.
The scalp: A problem people rarely connect
Most people don’t think of the scalp as an acne zone — but it can also be affected, and fungal vs bacterial acne on the scalp is a comparison that may be useful to understand, especially for anyone experiencing hairline breakouts or persistent scalp irritation.
Bacterial scalp acne tends to produce isolated tender pimples or pustules, often along the hairline or beneath the hair. Fungal scalp folliculitis presents as small, itchy, uniform clusters — sometimes accompanied by flaking not unlike dandruff. This isn’t coincidental. Malassezia is also associated with seborrhoeic dermatitis, so the two conditions can appear together.
Heavy, oil-based hair products are frequently a hidden driver here. Certain fatty acids — found in coconut oil, olive oil, and various other plant-derived oils — are known to feed Malassezia. If your scalp breaks out more after using particular products, it’s worth examining the ingredient list with that in mind.
Your moisturiser might be the problem
This is where skincare choices get personal, and potentially counterproductive.
Malassezia feeds on certain fatty acids. Many popular, well-reviewed moisturisers contain these fatty acids — coconut oil, olive oil, sunflower oil, and certain esters appear frequently in conventional skincare. For someone with bacterial acne, these ingredients might be fine. For someone with fungal acne, they may contribute to ongoing symptoms while limiting the effectiveness of other treatments.
Finding a fungal and bacterial acne safe moisturiser means looking for products that are lightweight, non-comedogenic, free of the oils most associated with Malassezia overgrowth, and ideally fragrance-free. Gel-based formulas may be suitable for many people. Squalane is generally considered safe. Ingredients like niacinamide, zinc, and hyaluronic acid tend to be tolerated well across both conditions — they support the skin barrier without feeding yeast.
If you’re currently unsure which type of acne you’re dealing with, this may be a practical initial step: simplify your moisturiser. Strip it back to something minimal and oil-free while you figure out what’s actually going on.
Treatment: Getting it wrong has real consequences
Bacterial acne is treated with antibacterial approaches — benzoyl peroxide, topical antibiotics, retinoids, and for more severe cases, oral medications. These have a solid track record, and a dermatologist can map out the right pathway based on severity.
Fungal acne may not respond to these treatments. This distinction is clinically important — antifungals are typically used. Topical ketoconazole and selenium sulfide shampoo (used as a body wash) are commonly recommended starting points. In persistent cases, oral antifungals may be necessary.
Here’s the part that genuinely frustrates people once they find out: oral antibiotics don’t just fail to treat fungal acne — they may worsen symptoms in some cases. By killing off the bacteria that normally compete with Malassezia, antibiotics give the yeast an open field. Someone prescribed antibiotics for what they assume is bacterial acne, but is actually fungal, may experience worsening symptoms and blame themselves for it.
Months can pass this way. This may lead to frustration and delayed improvement. And the fix, once the right diagnosis is made, may be more manageable once correctly identified.
Side by side: The key differences
| Feature | Bacterial Acne | Fungal Acne |
| Appearance | Mixed — blackheads, cysts, papules | Uniform small bumps, all roughly the same size |
| Itchiness | Uncommon | Frequently present |
| Common zones | Face, back, chest | Forehead, cheeks, back, chest, scalp |
| Triggered by | Hormones, bacteria, clogged pores | Heat, sweat, antibiotics, heavy products |
| Responds to antibiotics | Yes | No — often worsens |
| Responds to antifungals | No | Yes |
The skin deserves the right diagnosis
Mixing up these two conditions is genuinely easy to do. The breakouts overlap visually, they show up in the same places, and neither one announces itself clearly. But the treatments are not interchangeable — and using the wrong one may delay appropriate treatment, it can set your skin back in ways that take months to undo.
If your breakouts are itchy, unusually uniform, and haven’t responded to conventional treatments, consider reassessing your current approach . Reassess your products, and consider the possibility that the problem might be fungal rather than bacterial. A skin scraping or simple clinical examination may assist in distinguishing between the two. If you’re in Australia and want a professional opinion as an alternative access option, Acne Express connects you with Fellows of the Australasian College of Dermatologists via telehealth — with after-hours and weekend appointments available. A GP referral may make you eligible for a Medicare rebate. Accessing assessment may be more straightforward with appropriate services.
The right diagnosis, honestly, plays an important role in management.
Disclaimer: This article is for general informational purposes only and does not constitute medical advice. For persistent or severe skin concerns, please consult a qualified dermatologist or healthcare professional.